What you need to know
Slit Lamp Viewing:
• Diffuse beam • Medium magnification (around 16x) • 2 drop instillation of Lissamine Green and observe 1-5 mins later; or 2 drop instillation of fluorescein and observe with cobalt blue filter 3- 5 mins later
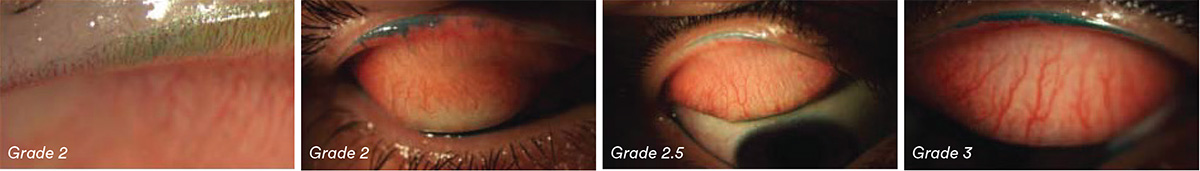
Grading:
Mean of grade for staining length (mm) and grade for sagittal width of staining (% of width of wiper area)
0: <2mm horizontal length of staining
1: 2-4mm horizontal length of staining
2: 5-9mm horizontal length of staining
3: >9mm horizontal length of staining
0: <25% average sagittal width of staining
1: 25-50% average sagittal width of staining
2: 50-75% average sagittal width of staining
3: >75% average sagittal width of staining
Incidence:
- Up to 85% of habitual soft lens wearers
- 88% of non-CL wearers with dry eye symptoms (32% ≥ grade 2) and 16% of asymptomatic non-wearers
- Can occur in the absence of positive dry eye test findings
- Correlates with lid parallel conjunctival folds (LIPCOF), tear film stability and tear volume, mucin quantity, bulbar and limbal hyperaemia, ocular surface staining and dry eye symptoms
- More common with rigid corneal (RCL) and SiHy lenses
Aetiology:
- Alteration in epithelium of advancing lid margin due to friction during lid movement across the lens surface
- In dry eye, tear film thickness insufficient to separate ocular surface and lid wiper
- Other causes include blinking disorders, lid and ocular surface abnormalities
Symptoms:
- Increased lens awareness
- Scratchiness on blinking
- Reduced wearing time
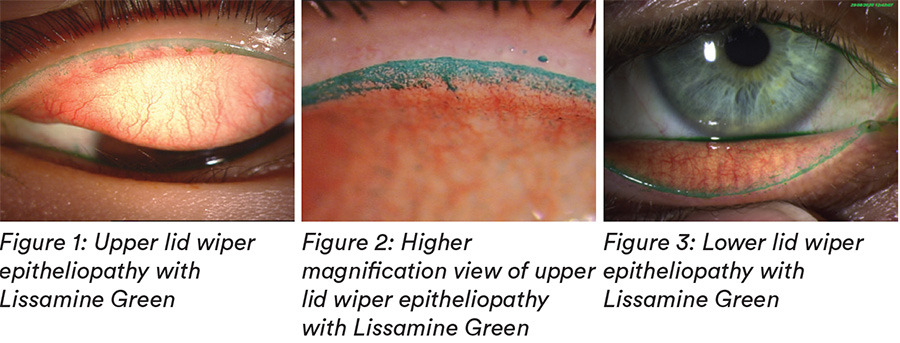
Signs:
- Characteristic staining at upper lid margin
What you need to recommend to your patients
Management:
- Manage ≥ grade 2 or if symptoms present
- Refit with more lubricious lens surface (lower coefficient of friction)
- Change lens type (rigid corneal (RCL) to hydrogel, or SiHy to hydrogel) or wearing schedule (increase replacement frequency)
- Maintain good lens cleaning including rub and rinse step
- Manage any tear quality issues
- Rewetting drops
Prognosis
Generally good resolution of symptoms with appropriate management, although signs may remain.
Differential diagnosis
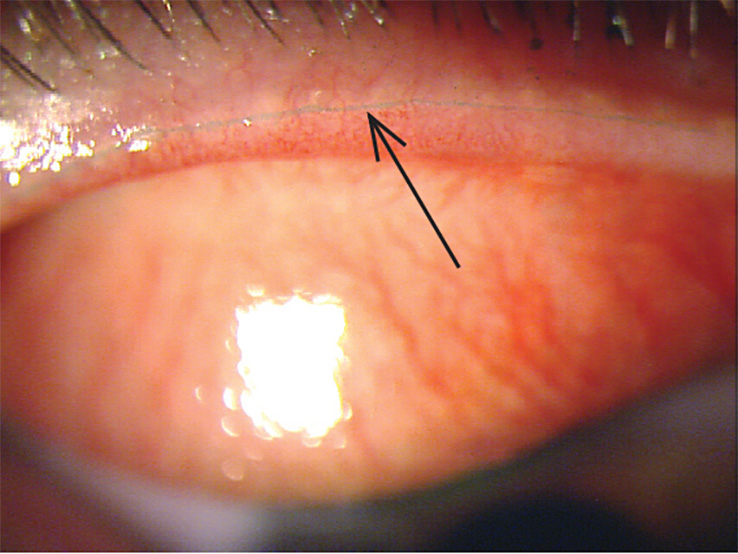
Staining associated with Marx line (above) and true lid wiper staining
Further reading
- Berry M et al. Mucins and ocular signs in symptomatic and asymptomatic contact lens wear. Optom Vis Sci 2008; 85(10): E930-8
- Doughty M et al. Visualisation of “Marx’s line” along the marginal eyelid conjunctiva of human subjects with lissamine green dye. Ophthalmic Physiol Opt 2004; 24(1): 1-7
- Efron N et al. Lid wiper epitheliopathy. Prog Retin Eye Res 2016; 53: 140-74.
- Knop E et al. The lid margin is an underestimated structure for preservation of ocular surface health and development of dry eye disease.
- Dev Ophthalmol 2010; 45: 108-22
- Korb D et al. Lid-wiper epitheliopathy and dry-eye symptoms in contact lens wearers. CLAO J 2002; 28(4): 211-6
- Korb D et al. Lid wiper epitheliopathy and dry eye symptoms. Eye Contact Lens 2005; 31(1): 2-8
- Korb D et al. Prevalence of lid wiper epitheliopathy in subjects with dry eye signs and symptoms. Cornea 2010; 29(4): 377-83
- Lievens C et al. Optimal methodology for lid wiper epitheliopathy identification. Cont Lens Ant Eye 2020; S1367-0484(20)30099-0
- Lin M et al. Mechanical complications induced by silicone hydrogel contact lenses. Eye & CL 2013; 39(1): 115–124
- McMonnies C. Incomplete blinking: exposure keratopathy, lid wiper epitheliopathy, dry eye, refractive surgery, and dry contact lenses. Cont Lens Ant Eye 2007; 30(1): 37-51
- Muntz A et al. Cytomorphological assessment of the lid margin in relation to symptoms, contact lens wear and lid wiper epitheliopathy. Ocul Surf 2020; S1542-0124(19) 3030: 1-5
- Pult H et al. The relationship between clinical signs and dry eye symptoms. Eye 2011; 25(4): 502-10
- Schulze M et al. Lid Wiper Epitheliopathy in Soft Contact Lens Wearers, Optom Vis Sci 2016 August; 93(8): 943-954
- Varikooty J et al. Atypical manifestation of upper lid margin staining in silicone hydrogel lens wearers with symptoms of dry eye. Cont Lens Ant Eye 2008; 31(1): 44-6
- Yeniad B et al. Lid- wiper epitheliopathy in contact lens users and patients with dry eye. Eye Contact Lens 2010; 36(3): 140-3
- Click here to review our Slit Lamp Techniques Videos
Patient case study
When you have read this guide and our recommended resources, why not take part in the Johnson & Johnson Institute self-assessment quiz to test your clinical, diagnostic and management skills. Choose only one answer to each question then check the answers at the foot of the page to see whether it’s correct. Good luck!
History
Patient AS is 36 years old and works long, irregular hours in a call centre. He has worn monthly replacement silicone hydrogel contact lenses for 7 years. Six months after his aftercare appointment he returns complaining that his lenses are ‘scratchy’ on blinking and his maximum comfortable wearing time is 6 hours.
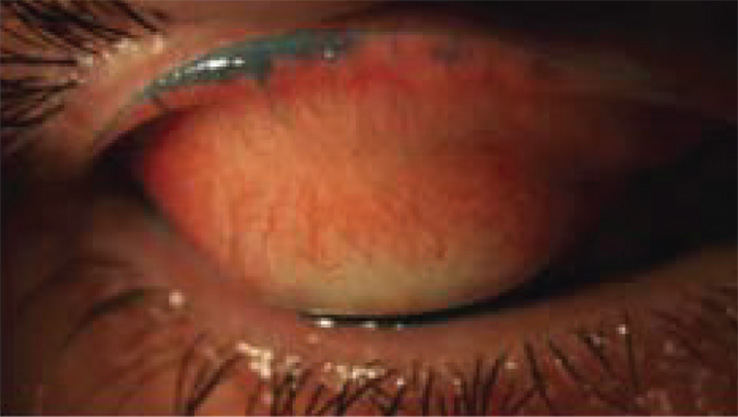
Questions
1. What is the best staining technique for examining this patient’s lid margin?
A. Fluorescein followed by lissamine green
B. Lissamine green only
C. Fluorescein only
D. Rose bengal only
2. What grade would you give to his LWE?
A. Grade 0
B. Grade 1
C. Grade 2
D. Grade 3
3. What proportion of contact lens wearers with dry eye symptoms show LWE on staining?
A. 68%
B. 78%
C. 88%
D. 98%
4. Which of the following management options could you consider?
A. Discontinue lens wear
B. Continue with current lenses and reduce wearing time
C. Refit with RGPs
D. Switch to silicone hydrogel lenses with a more lubricious lens surface and shorter replacement schedule
Answers
1. Correct answer is A. To examine the lid wiper area use fluorescein and cobalt blue illumination then lissamine green and white light
2. Correct answer is C. Grade 2. About 50-75% of the sagittal width of the lid wiper shows staining so this would be a Grade 2 LWE
3. Correct answer is C. LWE is a very common finding in contact lens wearers experiencing dryness and also in non-wearers with dry eye symptoms
4. Correct answer is D. LWE grade 2 or over, or with symptoms, needs to be managed. Refit with lenses of a lower coefficient of friction and shorter replacement